Table of Content
- Patient-Driven Groupings Model (PDGM)
- What Is the Medicare Deductible?
- HOME AND COMMUNITY-BASED SERVICE - State
- What is Telehealth, Telemedicine, and Remote Patient Monitoring?
- $1.7T spending bill eases Medicare rate cuts, extends telehealth waivers
- Reimbursement
- Ivy Rehab Network Physical Therapy and Rehab Professionals
- How Much Can You Make And Qualify For Medicaid
As part of the overall reimbursement cuts, CMS is proposing a 7.69% rate cut to reflect their calculations on behavioral adjustments. These adjustments are intended to account for the actual vs assumed behavior changes on aggregate expenditures due to the switch from HH PPS to PDGM. Keep in mind this is a prospective rate cut starting in CY 2023, and does not address the overpayments from CY 2020 and CY 2021. ADA DISCLAIMER OF WARRANTIES AND LIABILITIES. CDT-4 is provided "as is" without warranty of any kind, either expressed or implied, including but not limited to, the implied warranties of merchantability and fitness for a particular purpose.

CMS this month proposed establishing special enrollment periods for people who lose Medicaid or CHIP benefits because their income rose during the pandemic. States had expected to resume eligibility checks once President Joe Biden’s administration declared an end to the COVID-19 public health emergency. An estimated 18 million individuals could lose coverage when states start reviewing patients’ eligibility for Medicaid and the Children's Health Insurance Program, according to a December report from the Robert Wood Johnson Foundation. Local officials promised to pause trimming their public benefit rolls during the emergency declaration period in exchange for federal COVID-19 relief.
Patient-Driven Groupings Model (PDGM)
AHA said that the 2.7 percent Medicare reimbursement update for home health agencies does not accurately reflect the financial challenges that home health agencies have faced during the pandemic. As of January 2022, HHAs now need to complete and submit a notice of admission to their MAC within five days of starting a patient’s home health episode. You will need to consistently provide all documentation and consolidated billing for Part A and Part B services to your Medicare Administrative Contractor to receive efficient reimbursements. Preventive services for early detection of illness are also included under the Part B episode of Medicare benefits.

You must also continue to pay your monthly Medicare Part B and Part D premiums. Your dialysis facility must provide these items and services, either directly or through an arrangement with another provider. To qualify for a home health benefit from the US Center of Medicare & Medicaid Services , you need to consider the type of services your HHA provides to patients. According to estimates from a McKinsey study, $265 billion worth of care services for Medicare fee-for-service and Medicare Advantage beneficiaries could shift from traditional facilities to at-home care by 2025.
What Is the Medicare Deductible?
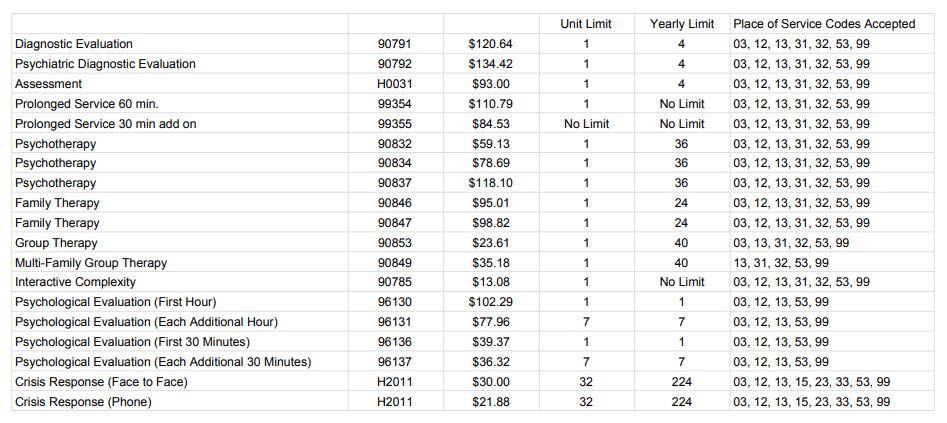
Payment for a 60-minute, 4-unit physical therapy treatment under Medicare part B averages between $97 and $105 on average. Because of how much the evaluation code is worth, the first visit costs between $130 and $160. Data from the Centers for Medicare & Medicaid Services indicates that Medicare normally covers about 80% of costs.
No fee schedules, basic unit, relative values or related listings are included in CDT-4. The ADA does not directly or indirectly practice medicine or dispense dental services. The sole responsibility for the software, including any CDT-4 and other content contained therein, is with or the CMS; and no endorsement by the ADA is intended or implied. The ADA expressly disclaims responsibility for any consequences or liability attributable to or related to any use, non-use, or interpretation of information contained or not contained in this file/product. This Agreement will terminate upon notice to you if you violate the terms of this Agreement.
HOME AND COMMUNITY-BASED SERVICE - State
The omnibus bill, which requires the approval of the House and Senate, has to be approved by the end of Friday or the government faces a potential shutdown. Moreover, if you’re social security recipient, your premiums restrict from rising under the Medicare hold harmless provision ruling. However, they may potentially involve different financial risks or value-based reimbursement structures. Moreover, if youre social security recipient, your premiums restrict from rising under the Medicare hold harmless provision ruling. Although income eligibility varies with State, the basic rule is that legal residents of the US with income 138% below the poverty line can qualify for Medicaid. Moreover, depending on the eligibility criteria, you can have both Medicaid and Medicare.
Neither of those statements are accurate, at least not according to our experience. Covered lives assessments are based on the HCRA region in which the member resides and the member’s enrollment status . Surcharges and covered lives remittances are required monthly, accompanied by the Certification Form, Report of Patient Services Payments and Surcharge Obligations, and Report of Covered Lives Assessments . The Indian Health Service rate is an all-inclusive rate reimbursed to IHS and tribal facilities by CMS for Medicaid-covered services.
What is Telehealth, Telemedicine, and Remote Patient Monitoring?
CPT is provided "as is" without warranty of any kind, either expressed or implied, including but not limited to, the implied warranties of merchantability and fitness for a particular purpose. AMA warrants that due to the nature of CPT, it does not manipulate or process dates, therefore there is no Year 2000 issue with CPT. AMA disclaims responsibility for any errors in CPT that may arise as a result of CPT being used in conjunction with any software and/or hardware system that is not Year 2000 compliant. No fee schedules, basic unit, relative values or related listings are included in CPT. The AMA does not directly or indirectly practice medicine or dispense medical services. The responsibility for the content of this file/product is with CGS or the CMS and no endorsement by the AMA is intended or implied.

The NADAC rate list is updated weekly to account for changing market prices as well as additions and deletions of NDCs. With US Legal Forms, you can easily create legally binding documents based on internet templates. If you have a problem finding a dialysis facility that’s willing to take you as a patient, you have the right tofile a complaint. Dialysis treatments from a Medicare-certified dialysis facility when traveling in the U.S. While this spells good news for your home health agency , it has never been more crucial for you to stay on top of the reimbursement process to maintain a healthy bottom line and revenue cycle. Before sharing sensitive information, make sure you’re on a federal government site.
Now that you have a basic know-how of both the programs lets delve into medicaid vs medicare reimbursement rates criterion. CMS projects that Medicare payments to HHAs in CY 2018 will be reduced by 0.4 percent, or $80 million, based on the finalized policies. Although the national average for home health aide pay in 2022 is $21 per hour, this number might vary widely from state to state. Fee-for-service Medicaid reimburses providers based on the number of patient visits. Fee-for-service Medicaid models allow states to choose their own reimbursement rates, but lawmakers in such states must still use federally mandated methodology.

After you pay the Part B yearly deductible, Medicare pays 80% of the monthly amount. In some cases, your doctor may be paid per day if you get services for less than one month. Or have a Medicare Supplement Insurance policy that covers all or part of your 20% coinsurance, then your costs may be different. Read your plan materials or call your benefits administrator to get your cost information.







